Measurement-Based Care (MBC) stands as a pivotal approach in mental health, aiming for enhanced precision and consistency in disease assessment, tracking, and treatment to achieve optimal outcomes. According to Harding and colleagues, MBC involves the systematic use of symptom rating scales to guide clinical decision-making, seeking to optimize accuracy and efficiency in symptom assessment.
Clinical Actionability and Symptom Rating Scales
For symptom rating scale data to be clinically actionable, it must be current, accurate, interpretable, and readily available during clinical encounters. Outdated symptom severity data, outside the context of the clinical encounter, lacks clinical actionability and is not considered effective MBC. The interpretability of symptom rating scale scores is crucial, with changes categorized to facilitate treatment guidelines and medication prescribing algorithms.
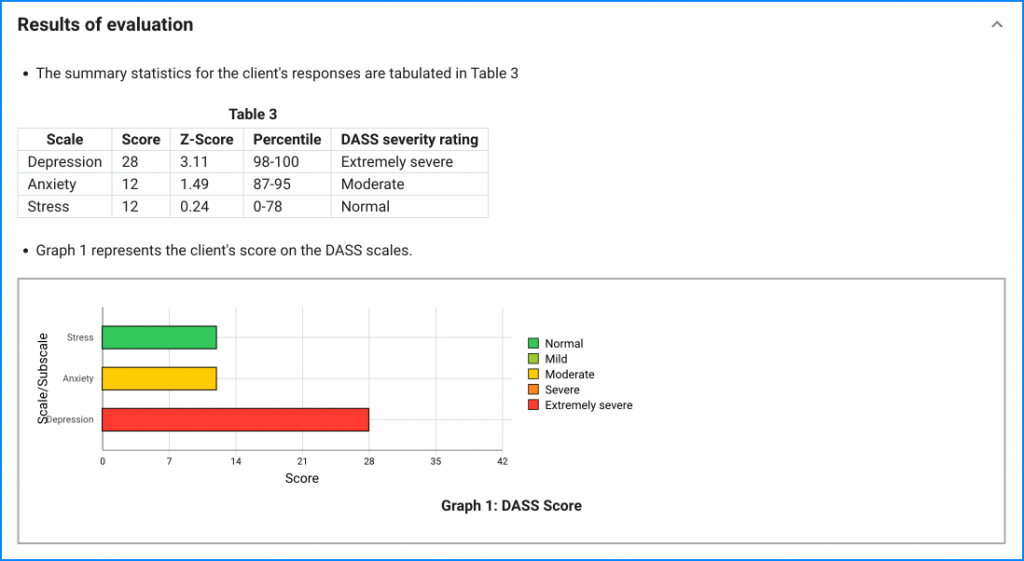
MBC and Depression Treatment Guidelines
Depression treatment guidelines recommend systematic reevaluation of symptoms at specified intervals. MBC greatly facilitates adherence to guidelines and algorithms by operationalizing and quantifying treatment responses. This approach supports the treat-to-target philosophy, emphasizing the revision of treatment plans until remission is achieved.
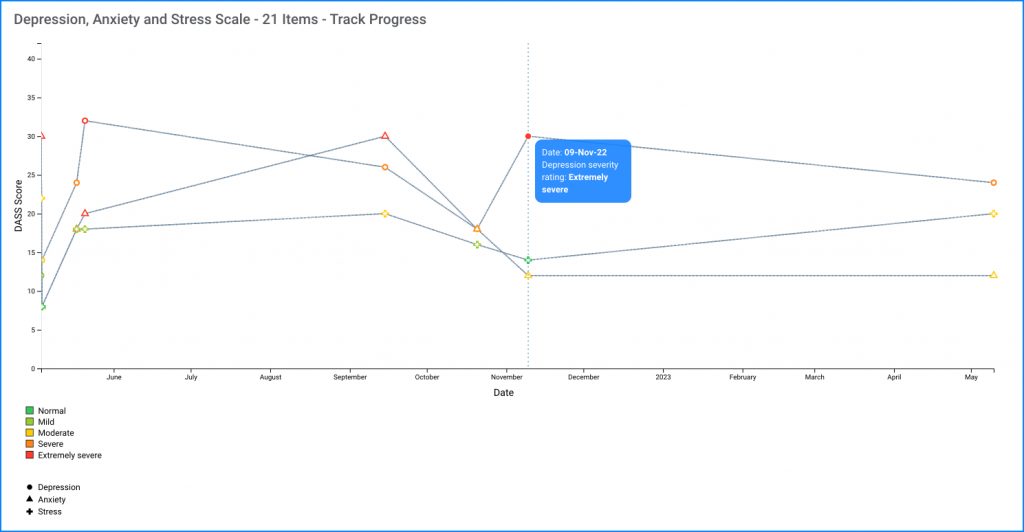
Residual Symptoms and Relapse Prevention
MBC plays a vital role in detecting residual symptoms, prompting clinicians to consider intensifying the treatment plan until complete remission. Residual symptoms, although not meeting diagnostic criteria, are linked to an increased risk of relapse. MBC aligns with collaborative care models, where self-reported depression severity scores are shared among care providers for team-based care.
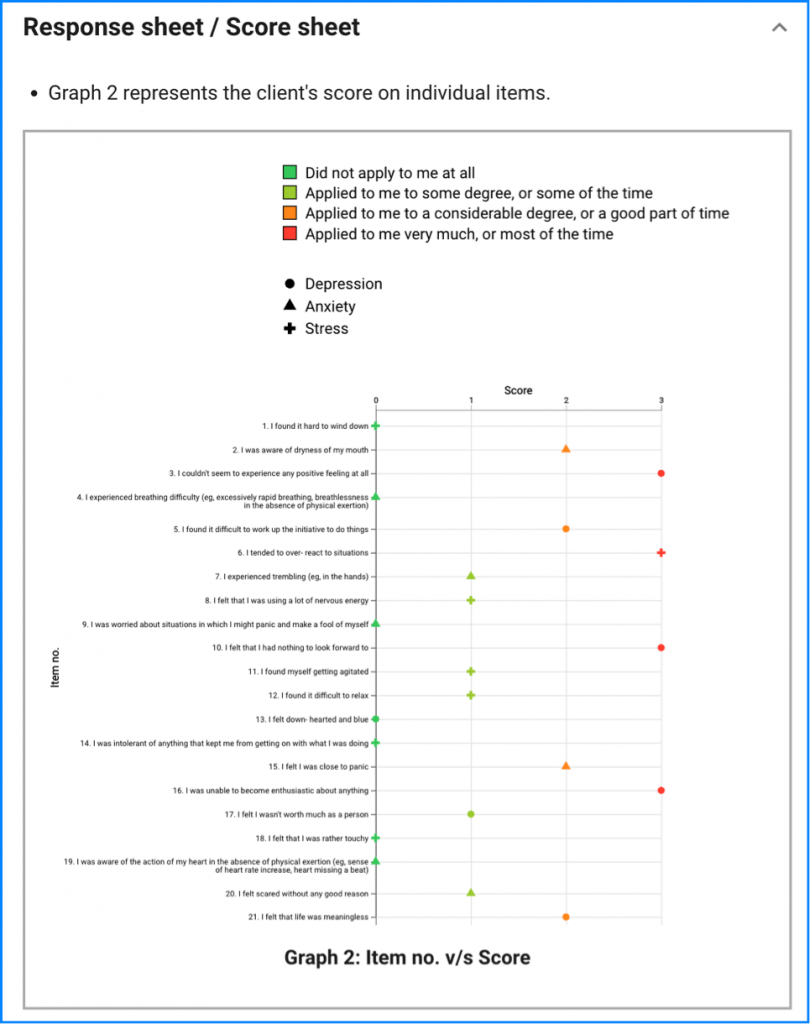
Enhanced Therapeutic Relationships and Patient Empowerment:
MBC contributes to more favorable patient outcomes by fostering enhanced therapeutic relationships and facilitating timely revisions of treatment plans. Patients regularly completing self-reported rating scales become more knowledgeable about their disorders, attuned to symptoms, and better equipped to self-manage their illness. Standardized symptom rating scales empower patients by involving them in clinical decision-making and validating their experiences.

Clinical Actionability and Sustainability
For MBC to be effective and sustainable, symptom severity feedback must be perceived as clinically actionable. The instruments used should be reliable and sensitive to change, ensuring consistent and meaningful measurements. Patient-reported outcomes serve as a starting point in evaluating the clinical effectiveness of current treatments.
Conclusion
In conclusion, MBC emerges as a transformative approach in mental health, not as a replacement for clinical judgment but as a tool to optimize the accuracy of assessments. By focusing on clinical actionability, interpretability, and sustainability, MBC stands as a powerful ally in the journey toward optimal mental health outcomes.
